News Letter, Vol. 3 (3), March, 2011, © Copyright
Jun Xu, M.D. Lic. Acup., Hong Su, C.M.D., Lic. Acup.
Robert Blizzard III, DPT
Rehabilitation Medicine and Acupuncture Center
1171 East Putnam Avenue, Building 1, 2nd Floor
Greenwich, CT 06878
Tel: (203) 637-7720
Hip Pain and Osteoarthritis
Luke L, a moderate obese, 45-year-old male had pain in his right hip for five years. The pain was of gradual onset and it sometimes radiates down through his right groin and right lateral thigh. He feels stiff and tight, and has difficulty walking and climbing the stairs. When in college, Luke was a football player, and now he still plays a lot of tennis and running. He sometimes felt pain in his right hip, however, he did not pay much attention to it. Over the last five years, the pain has intensified and recently becomes worse, to the extent of disturbing his sleep and limiting him to the point where he could only walk for a short distance.
He first consulted an orthopedic doctor who ordered an X-ray, which showed the joint space was narrowing with bone spur and subchondral sclerosis.
His doctor told him this was typical osteoarthritis of the hip, and, because the pain was so severe, Luke was given one steroid injection right away. He felt better for two months, but the effects of the shot wore off and the pain once again became worse. He returned to his orthopedic doctor and received second steroid injection. His orthopedic doctor told him that he probably needed a total hip replacement. As Luke is only 45 years old, he is reluctant to have the hip replacement, therefore, he consulted me.
On examination, I noticed when he walked he had a short swing of his right leg and he only could bear his weight on right leg with very short time, the short swing and stance phase on the affected side is called antalgic gait. In checking his range of motion, there appeared to be decreased external and internal rotation of the hip and the pain is elicited on the range of motion. An X-ray confirmed that Luke had severe osteoarthritis of the right hip.
There are different causes for hip osteoarthritis, however, the most common cause is secondary (i.e. from an injury).
- Primary osteoarthritis is aging related osteoarthritis. With aging, the water content of the cartilage increases, and the protein makeup of cartilage degenerates. After a certain period, the water content might also “dry out” after the cartilage gradually disappears, eventually, cartilage begins to degenerate by flaking or forming bone spurs. In advanced cases, there is a total loss of cartilage cushion between the bones of the joints.
- Secondary Osteoarthritis, i.e. the Repetitive use of the worn joints over the years, such as runners, tennis players, mountain climbers and martial art performers, etc, can irritate and inflame the cartilage, causing joint pain and swelling. Loss of the cartilage cushion causes friction between the bones, leading to pain and limitation of joint mobility. Inflammation of the cartilage can also stimulate new bone outgrowths (bone spurs, also referred to as osteophytes) to form around the joints. Osteoarthritis occasionally can develop in multiple members of the same family, implying a hereditary (genetic) basis for this condition. The following are the secondary causes of hip osteoarthritis
1. Sports or other sports-related injuries such as Luke’s – who was a marathon runner, who spent much time running– gradually changed the alignment of the hip and eventually leads to wear and tear on the joint surfaces.
2. Avascular necrosis. Many patients who drink alcohol excessively, and undergo steroid injections at the hip joint or took oral steroid for long period of life time, such as Lupus, or organ transplant recipients, might experience this condition, avascular necrosis is a death of the femoral head without sepsis. This is caused by interruption of the vascular supply to the femoral head. Luke had two such injections, which may have caused worsening of the hip osteoarthritis and possible avascular necrosis.
3. There are other causes, such as obesity, trauma, surgery, gout, diabetes and high uric acid, all of which can cause osteoarthritis.
Fig 3.1
 Treatment of osteoarthritis depends on the stages of the condition and the age of the patient.
Treatment of osteoarthritis depends on the stages of the condition and the age of the patient.
In the early stages, the following are indicated:
1. Weight reduction and the avoidance of activities that exert excessive stress on the joint cartilage. For Luke this meant he needs to lose 30-40 pounds (he lost 35) and stop playing tennis and running. Instead he was encouraged to peddle a stationary bicycle and swim. He rode his bike about 45 minutes a day and swam 3-4 times a week, and these activities, plus the weight he lost, put much less strain on his hip.
2. Anti-inflammatory medications such as aspirin, acetaminophen and naproxen, also anti-inflammatory lotions, dicolfenac and pain patch, Flector may help to decrease pain.
3. Injections: Hyaluronic acid injection is a chemical which can work by temporarily restoration of the thickness of the joint fluid and allow better joint lubrication and impact capability. Steroid injections can decrease the inflammation, thereby decreasing the pain of the joint.
Ultrasound machine may clearly identify the space of the hip joint and your physician can easily insert the needle into the hip joint and make an accurate injection at the hip joint under the guidance of ultrasound machine. Therefore, if you consider an injection of the hip joint, you should ask your physician if he or she uses the ultrasound guided technique.
Fig 3.2
4. Physical therapy:
4-way Hip Exercises on Mat
Start off with 3 sets of 10 reps for 30 reps total. Next session try 2 sets of 15 reps, then after that session try 1 set of 30 reps. Continue to progress by adding an ankle weight such as 2.5# and work up again from 3 sets of 10, 2 of 15 to 1 of 30, finally progressing to a 5# ankle weight and repeat the repetition cycle.
Hip Flexion involves lying on your back with one knee bent and the working leg straight being lifted up to the height of the opposite knee than down slowly.
Hip Extension involves lying on your stomach and lifting one leg up about 10-12” then down slowly.
Hip Abduction and Hip Adduction both involve lying on your side. Hip Abduction involves the top leg being lifted up around 20” then down slowly. Hip Adduction involves crossing the top leg over the bottom leg and performing the exercise by lifting the bottom leg off the table about 10” then down slowly.
Fig 3.3
http://www.sportsinjuryclinic.net/cybertherapist/corestability.php
http://www.best-leg-exercises.com/ankle-weights.html
4-way Hip Exercises Standing
After building the strength to perform 5# for 30 reps continue to progress by performing the 4-way Hip Exercises Standing with a TheraBand working the same repetition scheme. Performing these exercises in standing offers numerous benefits; from closely mimicking functional activities of daily living to improving balance. You can have a chair for support, but gradual try not to hold on to it. By not holding the chair you will feel the additional benefit of the stabilizing muscles around the hip that is supporting the body being worked; as well as the leg with the TheraBand performing the movement.
The first two pictures shown are Hip Flexion then Hip Extension. The following two are Hip Abduction then lastly Hip Adduction Exercises.
Fig 3.4
http://www.runnersworld.com/article/1,7124,s6-241-286–13410-0,00.html
http://www.resistancetubes.com/exercises.html
Another two great exercises to include both help improve rotation in the hips are the Clam Shell and the Seated External Rotation Exercise. The Clam Shell can easily be performed with the 4-way Hip Exercises on the Mat. In this movement keep the feet together but rotate the top knee up then down slowly. A weight or TheraBand can easily be added to increase the difficulty of the movement.
http://blog.victoriawellness.com/tag/hip-abduction/
With the Seated External Rotation Exercise keep the knees close as you move the foot away from the other foot to help work such muscles as the piriformis.
http://www.runnersworld.com/article/1,7124,s6-241-286–13410-0,00.html
5. Arthroscopy. Arthroscopy of the hip is a minimally invasive, outpatient procedure that is relatively uncommon. The doctor may recommend it if the hip joint shows evidence of torn cartilage or loose fragments of bone or cartilage.
6. Osteotomy. The procedure involves cutting and realigning the bones of the hip socket and/or thighbone to decrease pressure within the joint. In some people, this may delay the need for replacement surgery for 10 to 20 years. Candidates for osteotomy include younger patients with early arthritis, particularly those with an abnormally shallow hip socket (dysplasia).
In late stage of hip osteoarthritis, the following is indicated:
Following the progress of osteoarthritis of the hip, when the patient has pain even at rest and difficulty walking upstairs, it is recommended that the patient use a cane and consult a surgeon about replacement of the hip joint. Total hip replacement is now performed almost as a matter of routine, which can bring dramatic pain relief and improved function. The followings are the surgical options of hip replacement.
1. Hemi-Arthroplasty
From: http://www.eorthopod.com/content/hemiarthroplasty-hip
- As its name implies, hemi, or “half” of an arthroplasty. This procedure is usually performed as treatment for a hip fracture. The femoral head, due to irreparable damage to the blood supply, yet the patient’s acetabulum (socket) is in good condition, and not in need of a prosthetic cup implant.
The fractured femoral head is removed, a corresponding head implant is inserted into the remained femur bone canal, reamed to accommodate a prosthetic stem. These parts are either cemented into place, or “press-fit” to stimulate bone in-growth into the prosthesis. It is a very stable combination, and allows for early mobilization of the typical elderly patient to reduce the risks of other medical complications.
2. Traditional Hip Replacement
http://www.hosmatnet.com/Joint.htm
Traditional total hip replacement surgery involves making a 10- to 12-inch incision on the side of the hip in order to dislocate the hip joint.
Once the joint has been opened up and the joint surfaces exposed, the ball at the top of the thigh bone, or femur is removed. A cup-shaped implant is then pressed into the bone of the hip socket. It may be secured with screws. A smooth plastic bearing surface is then inserted into the implant so the joint can move freely.
Next, the femur is prepared. A metal stem is placed into the femur, or the thigh bone, to a depth of about 6 inches. A metallic ball is then placed on the top of the stem. The ball-and-socket joint is recreated. The stem implant is either fixed with bone cement or is implanted without cement. Cementless implants have a rough, porous surface. It allows bone to adhere to the implant to hold it in place.
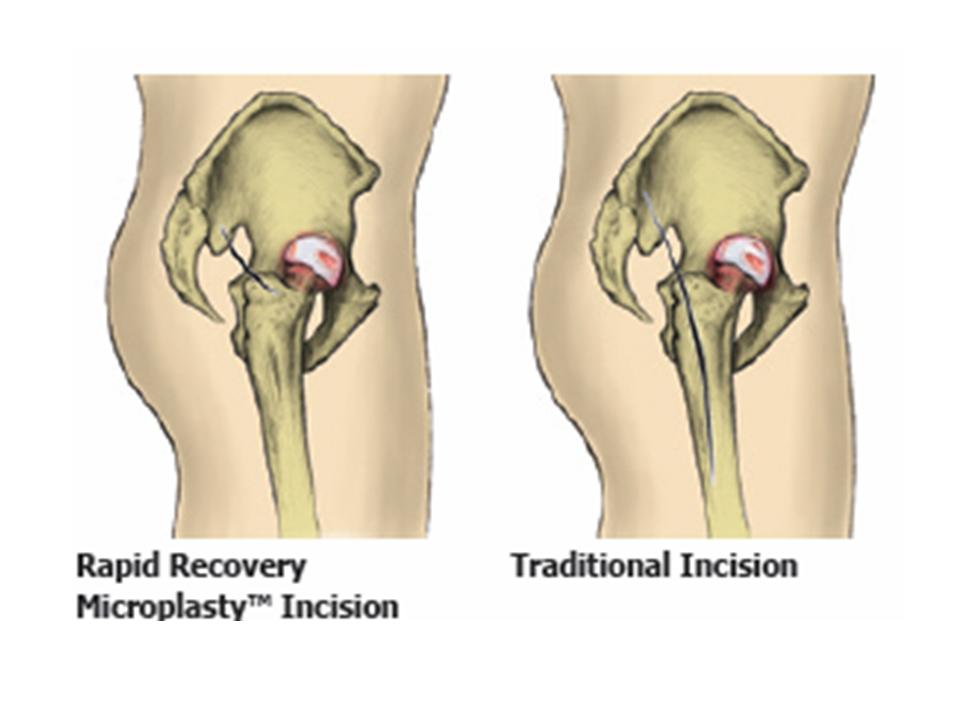
2. Minimally Invasive Hip Replacement
Fig 3.9
http://www.cleburneorthopedics.com/hip_replacement.html
Minimally invasive hip replacement surgery allows the surgeon to perform the hip replacement through one or two smaller incisions. Candidates for minimal incision procedures are typically thin, young, healthy individuals. The artificial implants used for the minimally invasive hip replacement procedures are the same as those used for traditional hip replacement. You should consult your orthopedic doctor for the possibility of this particular procedure. The benefit of the procedure are less pain, shorter hospital stay and better cosmetic and faster rehabilitation.
Treatment by traditional Chinese medicine:
Acupuncture must be combined with the above treatment to get better results. Acupuncture, as other treatments, can not prevent the arthritis develop further, however, acupuncture can dramatically decrease arthritic pain, decrease the swelling and inflammation, and effectively delay the surgical procedure.
There are two types of pathology of hip arthritis as per Traditional Chinese Medicine:
- Cold stasis: the typical symptoms are hip pain when the weather gets cold, windy or rainy. Many patients said: “ I do not need the weather man, I know it will be rainy or snow”. This is because the patients’ defensive system is not strong enough, weather changes make skin and joints sensitive, therefore, the invasive pathogens will be easier to get into the joints and make the joints stiff and pain.
- Hot stasis: the typical symptoms are swelling, hot and pain at the joints accompanied with low fever, red and painful touch at the joints, thirsty, annoy, depressed, constipated, hot urination, dry skin, wasted muscle, etc.
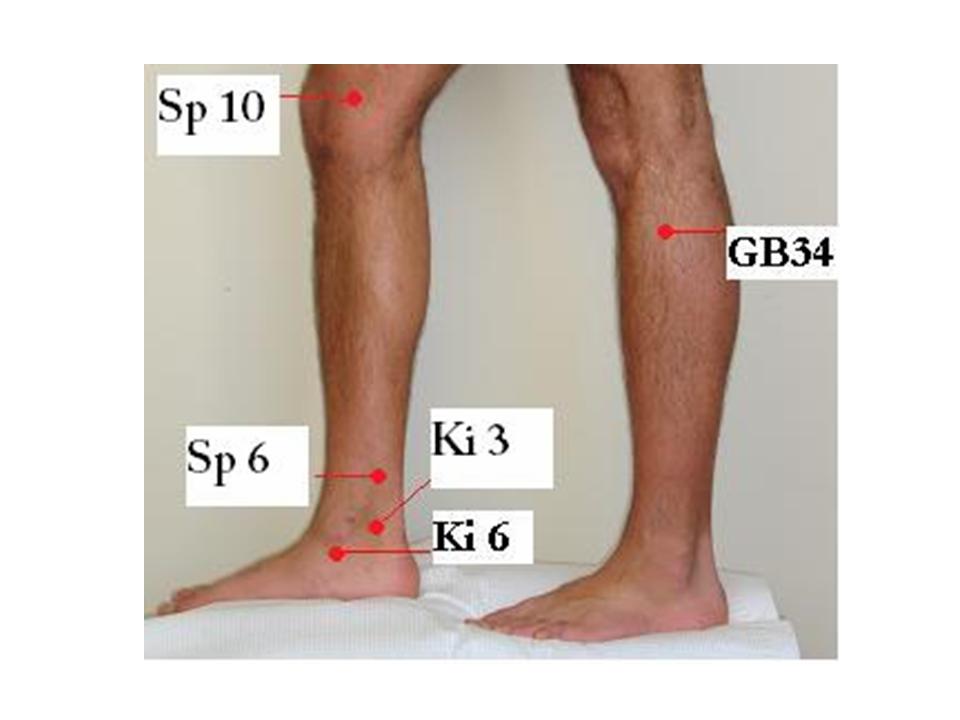
Acupuncture Points:
Main points: GB 30 Huan Tiao, GB 34 Yang Ling Quan, Arshi at the hip joint
Specific points for Cold Stasis: GB 20 Feng Chi, UB 18 Ge Shu, Sp 10 Xue Hai, Liv 3 Tai Chong, UB 23 Sheng Shu, Ren 4 Guan Yuan.
Specific points for Hot Stasis: Ren 6 Qi Hai, Sp 6 San Ying Jiao, Ki 3 Tai Xi, Du 14 Da Zhui.
| Points | Meridan/No. | Location | Function/Indication | |
| 1 | Huan Tiao | GB 30 |
At the junction of the lateral 1/3 between the great trochanter and the hiatus of the sacrum. |
Pain of the lumbar region and the thigh, muscular atrophy of the lower limbs, hemiplegia |
| 2 | Yang Ling Quan | GB 34 | In the depression anterior and inferior to the head of the fibula | Hemiplegia, weakness, numbness and pain of the knee, beriberi, hypochondriac pain, bitter taste in the mouth, vomiting, jaundice, infantile, convulsion |
| 3 | Feng Chi | GB 20 | In the depression between the upper portion of m. sternocleidomastoideus and m. trapezius, on the same level with Fengfu (Du 16) | Headache, vertigo, insomnia, pain and stiffness of the neck, blurred vision, glaucoma, red and painful eyes, tinnitus, convulsion, epilepsy, infantile convulsion, febrile diseases, common cold, nasal obstruction, rhinorrhea. |
| 4 | Ge Shu | UB 18 | 1.5 inch lateral to the midline, at the level of the lower border of the spinous process of the ninth thoracic vertebra | Jaundice, pain in the hypochondriac region, redness of the eye, blurring of vision, night blindness, mental disorders, epilepsy, back pain, spitting of blood, epistaxis |
| 5 | Xue Hai | Sp 10 | When the knee is flexed, 2 inch above the medial edge of patella. | Irregular menstruation, dysmenorrheal, uterine bleeding, amenorrhea, urticaria, eczema, erysipelas, pain in the medial aspect of the thigh |
| 6 | Tai Chong | Liv 3 | On the dorsum of the foot, in the depression distal to the junction of the first and second metatarsal bones. | Headache, dizziness and vertigo, insomnia, congestion, swelling and pain of the eye, depression,, infantile convulsion, deviation of the mouth, pain in the hypochondriac region, uterine bleeding, hernia, enuresis, retention of urine, epilepsy, pain the anterior aspect of the medial malleolus |
| 7 | Sheng Shu | UB 23 | 1.5 inch lateral to midline of spine at the level of the lower border of the spinous process of the second lumbar vertebrta | Nocturnal emission, impotence, enuresis, irregular menstruation, leucorrhea, low back pain, weakness of the knee, blurring of vision, dizziness, tinnitus, deafness, edema, asthma, diarrhea |
| 8 | Guang Yuan | Ren 4 | On the midline of the abdomen, 3 inches below the umbilicus | Lower abdominal pain, indigestion, diarrhea, prolapse of the rectum, enuresis, nocturnal emission, frequency of urination, retenstion of urine, hernia, irregular menstruation, dysmenorrheal, uterine bleeding, postpartum hemorrhage. |
| 9 | Qi Hai | Ren 6 | On the midline of the abdomen, 1.5 inch below the umbilicus | Abdominal pain, enuresis, nocturnal emission, impotence, hernia, edema, diarrhea, dysentery, uterine bleeding, irregular menstruation, dysmenorrheal, amenorrhea, morbid leucorrhea, postpartum hemorrhage, constipation, flaccid type of apoplexy, asthma |
| 10 | San Yin Jiao | Sp 6 | 3 inches directly above the tip of the medial malleolus, on the posterior border of the medial aspect of the tibiaFigure 24.22 | Abdominal pain, distension, diarrhea, dysmenorrheal, irregular menstruation, uterine bleeding, morbid leucorrhea, prolapse of the uterus, sterility, delayed labor, night bed wet, impotence, enuresis, dysuria, edema, hernia, pain in the external genitalia, muscular atrophy, motor impairment, paralysis and leg pain, headache, dizziness and vertigo, insomnia |
| 11 | Tai Xi | Ki 3 | In the depression between the medial malleolus and tendo calcaneus, at the level of the tip of the medial malleous.Figure 24.21 | Sore throat, toothache, deafness, tinnitus, dizziness, spitting of the blood, asthma, thirst, irregular menstruation, insomnia, nocturnal emission, impotence, frequency of micturition, low back pain. |
| 12 | Da Zhui | Du 14 | Below the spinous process of the seventh cervical vertebra, approximately at the level of the shoulders | Neck pain and rigidity, malaria, febrile diseases, epilepsy, afternoon fever, cough, asthma, common cold, back stiffness. |
Fig 3.10
Fig 3.11
Fig 3.12
Luke underwent my treatment so his pain temporarily decreased and the goal for this patient was to delay the total hip replacement procedure as long as possible. Therefore, Luke swims, rides his stationery bike and continues his weight loss, all of which put off the necessity of an operation for another two or three years.
Tips for patients:
1. Osteoarthritis of the hip is a progressive inflammation of the hip, for which there is no cure. Acupuncture can help – with other treatments –in delaying and decreasing the pain, however, the progress of worn cartilage is unpreventable.
2. For patients in their fourth or fifth decades, total hip replacement should be delayed as long as possible, because the mechanical joints usually last only about 15 years. If the patient undergoes this procedure too soon, you will expect to have it repeated in a decade and a half, so it would be best to put it off as long as is feasible. A second operation might increase the risks for surgery and its side effects.
3. Weight loss, swimming and peddling a stationery bicycle are the keys for the patient to help yourself. The patients should not perform the sports with high impact on the hip, such as running, jumping, etc.
Tips for acupuncturists:
1. There are many hip diseases that also cause pain, such as greater trochanteric bursitis, piriforms syndrome, iliopsoas bursitis and tendonitis, avascsualr necrosis of the femoral head and hip fractures, so it is important to properly differentiate among all the forms of hip pain.
2. You must differentiate the cold type from the hot one, because the treatments are different.