News Letter, Vol. 5 (3), March, 2013, © Copyright
Jun Xu, M.D. Lic. Acup. Hong Su, C.M.D. Lic. Acup.
Robert Blizzard III, DPT
Rehabilitation Medicine and Acupuncture Center
1171 East Putnam Avenue, Building 1, 2nd Floor
Greenwich, CT 06878
Tel: (203) 637-7720
Fax: (203)637-2693
Acupuncture and Perimenopausal Syndrome
Mary is a 48 year-old woman who complains of night sweats with poor sleep and hot flashes for last 4 months. She also notices irregular period that sometimes is very heavy in volume. She also notices the following symptoms of fatigue, mood swings, breast tenderness, decreased sex drive, vaginal dryness, discomfort during sex, urine leakage when coughing or sneezing along with urinary urgency. She consulted her primary care physician and was told to have perimenopausal syndrome. She was offered to take low dose birth control pills, or maybe estrogen replacement. She was afraid of the side effects of birth control pills and estrogen replacement, therefore, she comes to me for alternative treatment.
Mary has perimenopausal syndrome (PMS), which usually happens to women at age of around 45 years-old, however, each individual might have different experiences as some athletes start perimenopausal syndrome as early as 30 years-old with other women as late as age 60.
Menopause is defined as the state of an absence of menstrual periods for 12 months. The menopausal transition starts with varying menstrual cycle length and ends with the final menstrual period. Perimenopause is a term sometimes used and means “the time around menopause.” It is often used to refer to the menopausal transitional period. It is not officially a medical term, but is sometimes used to explain certain aspects of the menopause transition in lay terms.
Menopause is caused by the cessation of ovarian function. The ovary is a pair of reproductive glands in women. They are located in the pelvis, one on each side of the uterus. Each ovary is about the size and shape of an almond. The ovaries produce eggs (ova) and female hormones such as estrogen. During each monthly menstrual cycle, an egg is released from one ovary. The egg travels from the ovary through a Fallopian tube to the uterus.
The ovaries are the main source of female hormones, which control the development of female body characteristics such as the breasts, body shape, and body hair. The hormones also regulate the menstrual cycle and pregnancy. Estrogens also protect the bone. Therefore, a woman can develop osteoporosis (thinning of bone) later in life when her ovaries do not produce adequate estrogen.
Western Medicine Treatments
Estrogen Replacement Therapy (HRT)
Estrogen replacement therapy was a widely recommended treatment for menopausal symptoms as well as in the prevention of osteoporosis and heart disease.
Systemic estrogen replacement therapy (ERT) affects your entire body and reverses the effect of low estrogen. Systemic ERT may:
- Reduce the frequency and severity of hot flashes.
- Improve moodiness and sleep problems related to hormone changes.
- Maintain the lining of the vagina, reducing irritation.
- Increase skin collagen levels, which decline as estrogen levels decline. Collagen is responsible for the stretch in skin and muscle.
- Help prevent postmenopausal osteoporosis by slowing bone loss and promoting some increase in bone density.
- Reduce the risk of dental problems, such as tooth loss and gum disease.
Risks of estrogen replacement therapy
Estrogen replacement therapy (ERT) may increase the risk of health problems in a small number of women. This increase in risk depends on your age, your personal risk. Using ERT may increase your risk of:
- Stroke.
- Blood clots.
- Breast cancer.
- Gallstones.
- Ovarian cancer.
- Dementia.
Side effects that can occur with all forms of estrogen but are more common with oral estrogen (and less common with a patch, cream, gel, or vaginal ring) include:
- Headaches.
- Nausea.
- Vaginal discharge.
- Fluid retention.
- Weight gain.
- Breast tenderness.
- Spotting or darkening of the skin, particularly on the face.
- In rare cases, an increased growth of preexisting uterine fibroids or a worsening of endometriosis.
Some of these side effects, such as headaches, nausea, fluid retention, weight gain, and breast tenderness, may go away after a few weeks of use.
The estrogen patch (transdermal estrogen) may cause skin irritation.
An estrogen ring must be replaced every 3 months. If the ring falls out at any time during the 3-month treatment period, you may rinse it with lukewarm water and reinsert it.
Supplements, herbs and botanicals like black cohosh, evening primrose oil, and flaxseed are thought to relieve menopausal symptoms.
Black cohosh, also known as black snakeroot or bugbane, is a medicinal root. It is used to treat women’s hormone-related symptoms, including premenstrual syndrome (PMS), menstrual cramps, and menopausal symptoms.
Wild Yam and Progesterone Creams
Wild yam and progesterone creams are available without a prescription and are marketed for relieving perimenopausal symptoms caused by “estrogen dominance.”
Soy is high in isoflavones. Isoflavones are a type of phytoestrogen. Phytoestrogens are chemicals found in plants that work like estrogens.
Acupuncture and Chinese Herbs
Acupuncture treatment has long been used for perimenopausal symptoms (PMS), most Traditional Chinese Medicine physicians believe kidney deficiency is the main pathological cause for PMS. Therefore, acupuncture points selection is based on the above reasoning.
- Main points: Ren 4 Guan Yuan, Ren 3 Zhong Ji, Ren 19 Zi Gong, Sp 6 San Ying Jiao, Ht 7 Shen Men, Du 20 Bai Hui, Liv 3 Tai Cong, Pc 6 Nei Guan, Ren 17 Tan Zhong, GB 29 Ju Liao, and GB28 Wei Dao.
Here are some important points that must be used for PMS.
2. Accessory points: Kidney Yin Deficiency add points of Kid 10 Yin Gu, Ki 3 Tai Xi, Ki 12 Da He, UB 18 Gan Shu; Kidney Yang Deficiency add UB 20 Pi Shu, St 36 Zu San Li
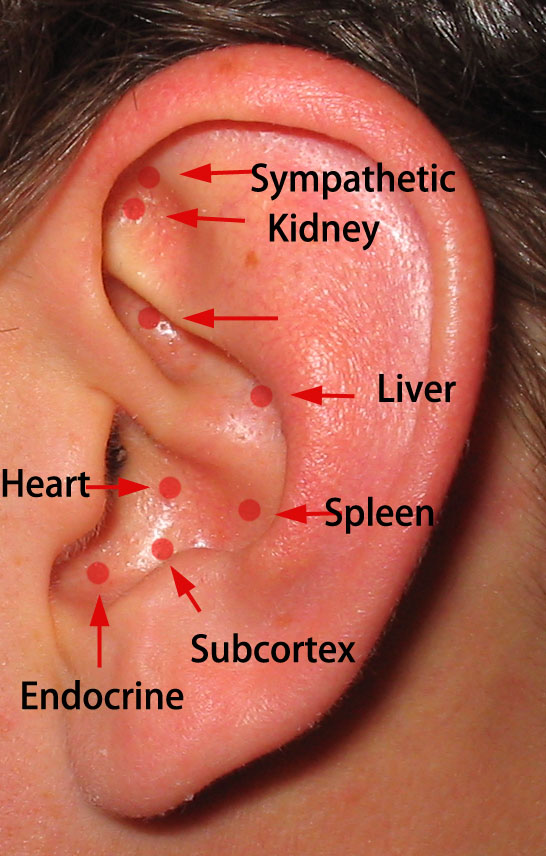
3. Ear Needles: Main Points, kidney, endocrine, sub-cortex, plus sheng meng, jiao gan, , liver, heart, spleen, etc.
Research evidence showed that PMS symptom was improved with decreased FSH, LF and increased E2 and endorphins level.
Acupuncture and many Chinese herb formulas have been used to effectively adjust the hormone level, the most important herbs are Bai Sa sheng, Mai Men Dong, Dan Gui, Di Huang, Gou Ji, Chuan Lian Zi, Ye Jiao Teng, etc. The formula prescribed depends on the diagnostic type of Chinese Medicine, each individual is different from other, therefore, no one formula can be used for all the patients without modification.
Mary’s Treatment
Mary was diagnosed of kidney deficiency, therefore, The main points were selected. However, Mary’s symptom also indicated liver yin deficiency, Liv 3 Tai Cong, UB 18 Gan Shu, Kid 3 Tai Xi were added to the treatment plan. She underwent acupuncture treatment 3 x per week for 4 weeks plus Chinese herb pills 2x per day, she felt much improved with her night sweats and hot flush, she also reported better sleep and less mood swing, she was continued to have acupuncture maintenance treatment once a week for 6 weeks, then she continued her Chinese herbs for rest of the treatment. After 4 months, she reported her symptom was almost gone.
Tips for the patients:
- The earlier, the better to get your treatment.
- Try to use both Chinese herbs and Acupuncture treatment.
- If it is possible, you should drink Chinese herb tea, which should be prescribed by physician who had really training. The formula should be individualized and based on your specific need.
- Keep smooth mood, always relaxed, do not put too much stress on yourself.
Tips for the acupuncturists:
- Chose some scalp points, such as Du 20 Bai Hui, GB 20 Feng Chi, Du 16 Feng Fu, GB 8 Shuai Gu, even Extra-point Tai Yang, will be very helpful.
- Try to use Chinese herbs to help, such as Gou Ji, Chuan Lian Zi, Yu Zhu, Shi Fu, let patient use them as tea.
- Stress reduction treatment is very important, the points in the liver meridian should be chosen, such as Liv 3 Tai Chong, Kid 3 Tai Xi, etc.