News Letter, October, 2014, © Copyright
Jun Xu, M.D. Lic. Acup., Hong Su, C.M.D., Lic. Acup.
James Olayos, DPT, CSCS
www.rmac.yourmd.com; www.drxuacupuncture.co
Rehabilitation Medicine and Acupuncture Center
1171 East Putnam Avenue, Building 1, 2nd Floor
Greenwich, CT 06878
Tel: (203) 637-7720
Frozen Shoulder and Acupuncture Treatment
From: www.1thing.info/50kata/gojukata1.gif
Martha T. is a 50-year-old woman with a long history of diabetes. Approximately two months before consulting me, she felt a slight pain in her right shoulder when she tried to lift a heavy object. Though the pain was not severe for the first few weeks, she gradually noticed a decrease in the mobility and function of that shoulder, coupled with more severe pain. After the incident, she had trouble lifting her arms for tasks such as combing her hair and dressing with ease, especially when putting clothes on her right arm or fastening her brassiere. Hoping the pain would go away, she did not consult a doctor.
When the pain became too severe, she came to me. By physical examination, I noted that there was moderate tenderness at the right frontal and posterior shoulder. Through palpation, I noted tenderness in her upper arm and lateral elbow. She had difficulty raising her right shoulder up to her head and with movements that crossed the body’s middle line. The pain was constant and she was unable to sleep on the right side of her body. Her right arm was weak due to the pain. There was no numbness or a tingling sensation.
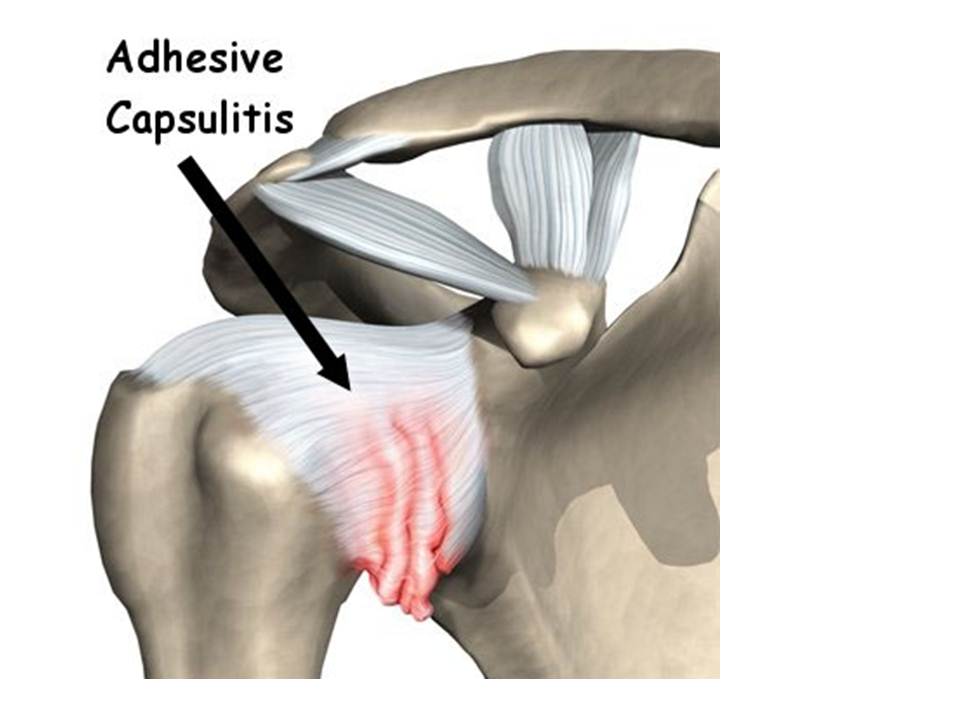
Martha suffers from a “frozen shoulder,” or, in medical terminology, adhesive capsulitis.
Fig. 1
This usually occurs after the age of 40, and about 20% of patients who suffer from this disorder have a history of diabetes and most of them have also been involved in some form of accident. When these patients begin to feel shoulder pain, they try to compensate by limiting the normal range of motion in the injured shoulder. Unfortunately, this makes some normal tasks such as brushing the hair, dressing, reaching for objects above the head, etc., more difficult. By this stage, the patient usually realizes it is necessary to seek medical treatment for the condition.
Frozen shoulder is usually exhibited in three stages:
- Painful stage: A gradual onset associated with a vague pain. Unknown specific date of onset. Lasts roughly 8 months.
- Frozen stage: The pain may begin to diminish during this stage. However, the shoulder becomes stiffer and the range of motion decreases noticeably, which causes the patient to avoid extreme movements that exacerbate the pain during this phase. Usually lasts from six weeks to nine months.
- Thawing stage: The shoulder movement gradually returns to normal and the pain lessens. Lasts from five months to two years.
Though the causes of frozen shoulder are still unclear, these are some noted possibilities:
- Injury resulting from surgery or any traumatic accident. Most patients have a history of an injury that causes pain and causes the patient to decrease his/her range of movements.
- Diabetic patients have a tendency to have frozen shoulder. In those patients who are diabetic (about 20%), this condition worsens the symptoms.
- Autoimmune, inflammatory, and any procedures that immobilize the shoulder will increase the chances of frozen shoulder.
Western medicine treatments:
- Anti-inflammatory medications: The use of anti-inflammatory medications such as ibuprofen, naproxen, etc. However, these oral medications are not a very effective treatment.
- Corticosteroid injection: Using a corticosteroid (i.e. 40 mg of Kenalog and 5 cc of 1% lidocaine injected directly into the shoulder bursa) will greatly decrease the intensity of the pain. However, there are some side effects of corticosteroid injections such as blood sugar elevation, fragile shoulder tendons, osteoporosis, etc. I usually do not recommend using corticosteroid injections unless it is absolutely necessary (i.e. when there is severe pain, largely decreased range of motion, and handicapped daily activities).
- Physical therapy: Using heating pads, stretching, performing wheel range of motion exercises, muscle strengthening, electrical stimulation, ultrasound, electrophoresis, etc. The dual treatment of corticosteroid injection and physical therapy can be very effective.
In some cases, surgery may be necessary. There are two common types of surgery used to treat frozen shoulder:
- Manipulation under general anesthesia: forces the shoulder to move. This process can unfortunately cause the capsule to stretch or tear.
- Shoulder arthroscopy: The doctor makes several small incisions around the shoulder capsule. A minute camera and instrument are inserted through the incision and the instrument is used to cut through the tight portion of the joint capsule. Often, manipulation and arthroscopic surgeries are used together and many patients have good results form this type surgery.
Physical Therapy Treatment for Frozen Shoulder:
Physical Therapy treatment generally begins in the first stage of the “frozen shoulder” progression. Upon initial PT evaluation of the effected shoulder, the therapist will begin with gentle passive and active range of motion activities within the patient’s pain tolerance. The primary goal in stages 1 and 2 of the frozen shoulder progression is to reduce pain and begin to regain normal joint motion. Passive stretching of the shoulder in all planes and manual joint mobilization techniques are indicated. Pain relieving modalities such as heat, electric stimulation, and short-wave diathermy can be used when it is at the therapist’s disposal. In addition, basic postural re-education exercises such as scapular retraction and pectoral stretching should be introduced.
Fig. 2
Fig. 3
Fig. 4
As the patient progresses from the “freezing” stage of the condition, more aggressive joint mobilization and stretching techniques are introduced to regain full motion of the shoulder joint. This stage can be painful at times, but it is necessary for long term results and return of normal function. Therapeutic exercises (shoulder elevation, rotation, scapular retraction against resistance, etc.) are progressed to allow for shoulder stabilization within the new ranges of motion achieved with stretching and joint mobilization.
During the final stage of the frozen shoulder progression, the therapist will introduce functional activities to ensure that the effected shoulder is prepared for daily tasks. Pain level should be decreased at this point in treatment.
Traditional Chinese Medicine Treatment:
The following points were selected:
LI 15 Jian Yu, SI 9 Jian Zhen, SJ 14 Jian Liao, SI 10 Nao Shu, SI 11 Tian Zhong, LI 16 Ju Gu, St 38 Tiao Kou penetrating to UB 57 Cheng Shan, SJ 5 Wai Guan and LI 4 He Gu, LI 11 Qu Chi.
Table 1
| Points | Meridian/No. | Location | Function/Indication | |
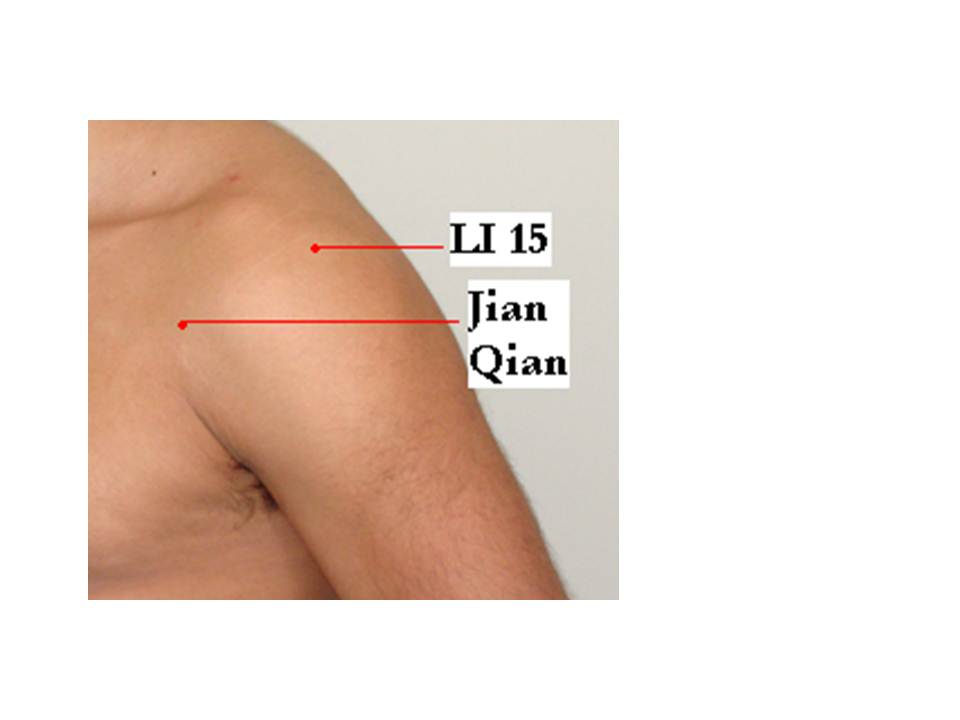
| 1 | Jian Qian | Extrapoints 23 | Midway between the end of the anterior axillary fold and LI 15, Jian Yu | Pain in the shoulder and arm, paralysis of the upper extremities |
| 2 | Jian Yu | LI 15 | See table 5-1/Pic 5-1 | See table 5-1 |
| 3 | Jian Zhen | SI 9 | Posterior and inferior to the shoulder joint. When the arm is adducted, the point is 1 inch above the posterior end of the axillary fold | Pain in the scapular region, motor impairment of the hand and arm |
| 4 | Jian Liao | SJ 14 | Posterior and inferior to the acromion, in the depression about 1 inch posterior to LI 15 Jian Yu, when the arm is abducted. | Pain and motor impairment of the shoulder and upper arm |
| 5 | Nao Shu | SI 10 | When the arm is adducted, the point is directly above SI 9 Jian Zhen, in the depression inferior to the scapular spine | Swelling of the shoulder, aching and weakness of the shoulder and arm |
| 6 | Tian Zhong | SI 11 | See table 5-1/Pic 5-2 | See table 5-1 |
| 7 | Ju Gu | LI 16 | In the upper aspect of the shoulder, in the depression between the acromial extremity of the clavicle and the scapular spine | Pain and motor impairment of the upper extremities, pain in the shoulder and back |
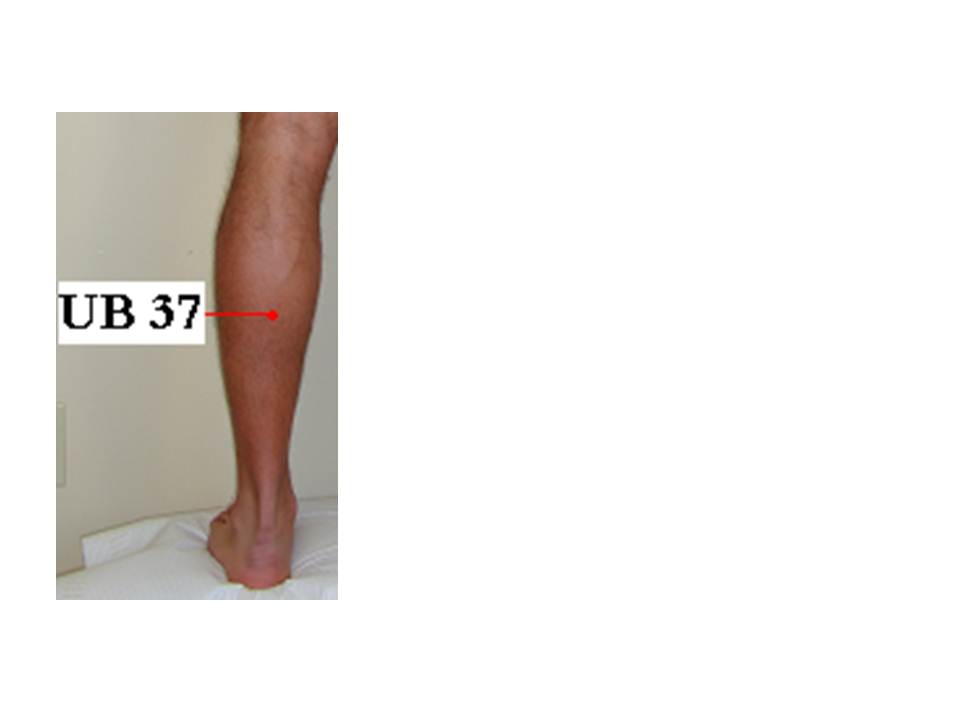
| 8 | Tiao Kou | St 38 | 2 inches below St 37 Shang Ju Xu, midway between St 35 Du Bi and St 41 Jie Xi. | Numbness, soreness and pain of the knee and leg, weakness and motor impairment of the foot, pain and motor impairment of the shoulder, abdominal pain |
| 9 | Cheng Shan | UB 57 | Directly below the belly of m. gastrocnemius, on the line joining UB 40 Wei Zhong and tendo calcaneus. About 8 inches below UB 40. | Low back pain, spasm of the gastrocnemius, hemorrhoids, constipation, beriberi |
| 10 | Wai Guan | SJ 5 | See table 5-1/Pic 5-3 | See table 5-1 |
| 11 | He Gu | LI 4 | See table 3-1/Pic 3-4 | See table 3-1 |
| 12 | Qu Chi |
Fig. 5
Fig. 6
Fig. 7
Fig. 8
To treat Martha, I applied the heating pad to her right shoulder for approximately 20 minutes. This increased the flexibility of the tendon underneath. Then, I inserted the needles into the above acupuncture points. After 30 minutes of acupuncture treatment, I gave her a deep massage, and she was told to raise her shoulder and perform other range of motion exercises. The patient underwent my treatment for a total of 10 visits. Afterwards, she reported that her right shoulder pain and range of motion had improved greatly.
Tips for acupuncturists:
- Instruct the patient to sit down and relax. First, insert the needle into the Qu Chi tips toward to the shoulder about 1.5 inches deep, causing the energy to transmit up to the shoulder. Then insert the needles into the points of Jian Yu, Jian Zhen, Jian Liao, and Tian Zhong. Insert the needle into Tiao Kou so that it penetrates to Cheng Shan. During the treatment, scratch the handles of needles, and make sure the patient feels this energy sensation from the needle tips spreading to the shoulder.
- Tell the patient to slowly raise his/her arm up to the head, and move the arm around. Usually, the patient will feel instant relief from the pain.
Tips for patients:
- Do range of motion exercises for 20 minutes every morning taking a hot bath or shower. The hot water increases the blood circulation and energy flow and will allow for the best range of motion and the least pain when doing these exercises.
- Purchase a heating pad and apply it to the shoulder for 20 minutes. Do the range of motion exercises again.
- The main goal is to increase the range of motion of the shoulder. The second goal is to decrease the pain in the shoulder.
- Try to get an acupuncture treatment as soon as possible; do not wait. Without treatment, it may take a few years for natural recovery, and in some cases range of motion will never fully return.