Dear Friends and Patients:
Time flies! Now it is the time for our news letter 6, bronchitis. You may find some useful info for your reference. So far, we have sent out total 6 news letters in this year. If you or your friends would like to read previous news letters, please visit: www.drxuacupuncture.co. You are welcome to forward our news letters to your friends. Here are the titles of all of the previous case discussions:
2. Headaches
4. Osteoporosis
5. Common cold
Thank you very much and have a wonderful July 4th!
Best wishes,
Jun Xu, M.D., & Hong Su Xu, C.M.D.
News Letter, Vol. 1 (6), June, 2009, © Copyright
Jun Xu, M.D. Lic. Acup., Hong Su, C.M.D., Lic. Acup.
www.rmac.yourmd.com; www.drxuacupuncture.co
Rehabilitation Medicine and Acupuncture Center
1171 East Putnam Avenue, Building 1, 2nd Floor
Greenwich, CT 06878
Tel: (203) 637-7720
Case Discussion: Bronchitis
Susan W., a 45-year-old female. came to my office complaining of a severe cough which had lasted for about three or four weeks. It caused her tremendous pain on her chest and abdominal muscle and she also coughed out yellowish greenish phlegm and sometimes experienced wheezing and shortness of breath; she also was running a low fever and had chills and muscle aches. She also suffered nasal congestion and sore throat and had difficulty swallowing food. Her ears were blocked, making it difficult to hear, and she was extremely uncomfortable in many areas when she came to me for evaluation and treatment.
This patient most likely had bronchitis, an irritation and inflammation of the airways. It is often triggered by the upper respiratory tract infection such as the common cold or influenza, and can also be caused by sinus infection, as well as exposure to irritating fume or dust or fur of cats or dogs or tobacco smoke. According to Western medicine, there are five types of bronchitis based on western medicine:
1. Acute bronchitis. It will last about several days to weeks and usually it will clear up on its own.
2. Viral bronchitis. This is triggered by viral infection such as common cold.
3. Occupational bronchitis. Patients are exposed to lung irritants in one’s home or work place and the treatment usually is withdraw from the place.
4. Chronic bronchitis. The above symptoms will last for longer than three months or recur at a frequency over period of years so this chronic bronchitis usually is not caused by infection but is very often associated with chronic obstructive pulmonary disorder.
5. Asthmatic bronchitis refers to the same symptoms but the underlying cause is asthma.
Traditional Chinese medicine believes bronchitis is a lung disease which results either from attack of the exogenous pathogenic factors or from disorders of the lung itself.
For the invasion of the exogenous pathogenic factors, there are two types:
1. Wind cold: The main manifestations are cough, itching in the throat, thick white sputum, and the patient is easily susceptible to cold, with symptoms such as fever, anihidrosis, headache, nasal obstruction and discharge with thin white tongue coating, and superficial pulse.
2. Wind heat: The main manifestations are choking cough with yellowish thick sputum, thirst, sore throat, fever, headache, and the patients are aversion to wind and with symptom of sweating, with thin yellow tongue coating and superficial and rapid pulse.
For the internal organ injury of the lung, there are two types.
1. Blockage of the lung by phlegm. The main manifestation is cough with profuse, thick white sputum and stuffiness and congestion of the chest, loss of appetite, white sticky tongue coating, and rolling pulse.
2. Dryness of the lung with deficiency of yin. This is manifested by dry cough without sputum or with scanty sputum, dryness of the nose and throat, sore throat, spitting – or even – coughing of blood, afternoon fever, malar flash, red tongue, with thick tongue coating, and rapid pulse.
Treatment:Western medicine.
By far the majority of bronchial cases are originally from viral infections, this means that most cases of bronchitis are short term and require nothing more than symptomatic treatment. Since antibiotics do not cure a viral illness, overuse of antibiotics will make the bacteria habituated in the respiratory tract resistant to the antibiotics currently available. Many doctors prescribe antibiotics because they feel pressure from the patients. If they do not prescribe certain antibody, then the patient will think the doctor did nothing to help.
We can use acetaminophen to control the fever, such as, Tylenol, aspirin, or ibuprofen. Also the patient should drink as much fluid as possible in order to clear the body, dilute the virus and to make the virus dissipate in the body’s fluid. A humidifier might also help and over-the-counter cough suppressants such as the Robitussin and Mucinex might also assist in loosening the secretions.
Bronchodilator inhalers will help open airways and decrease the wheezing. If there is bacterial infection, then antibiotics should be prescribed.
Traditional Chinese medicine and acupuncture treatments:
1. For wind cold. You may choose acupuncture points such as Lu 7 Lie Que, LI 4 He Gu, and UB13 Fei Shu (Lung Shu), and with supplementary points for pain and swelling of the throat, Lu11 Shao Shang, and for fever and aversion to cold Du14 Da Zhui and SJ 5 Wai Guan.
Pic 2-1
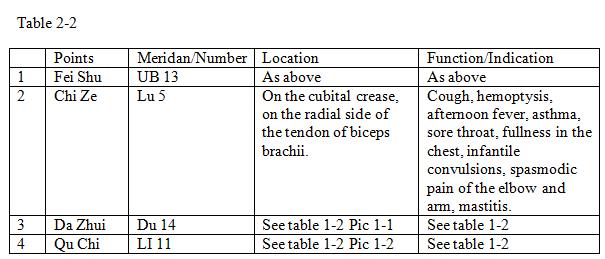
2. For wind heat: UB 13 Fei Shu, Lu 5 Chi Ze, Du 14 Da Zhui, LI 11 Qu Chi.
Pic 2-2
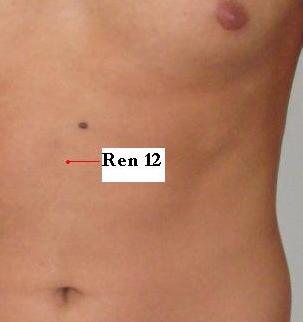
3. For the internal lung injury with the blockage of the lung by phlegm, so we select back-shu points and other lung points: like UB13 Fei Shu, Ren 12 Zhong Wan, Lu 5 Chi Ze, St 36 Zu San Li, St 40 Feng Long.
Pic 2-3 Pic 2-4
Acupressure tips for patients:
1. The most important points are Fei Shu, UB 13. Ask your friend or family member press the points on both side for 5 min each, alternately press until you feel energy flow go through your lung.
2. If you have fever or feel very cold, press Da Zhui, Du 14 for 10 min, then press Fei Shu. UB 13, which will greatly improve your immune ability and quickly decrease your cough and respiratory symptom, such as cough, sneeze, etc.
Acupuncture tips for acupuncture practitioners:
1. Always electrically stimulate Fei Shu , UB 13. If the patient has wind cold, Lie Que, Lu 7 and Da Zhui, Du 14; for wind heat, Qu Chi, LI 11 and Da Zhui, Du 14.
2. Combined Fei Shu, UB 13 with Zu Sanli St36 and Feng Long, St 40, you may greatly improve your patient’s immune function.
The above patient was diagnosed to have wind cold so after the treatment for about one week and her symptoms disappeared and she returned to work.